Diabetes Management
What is the Difference between Diabetes Insipidus and Diabetes Mellitus?
2 min read
By Apollo 24|7, Published on - 12 September 2023, Updated on - 14 September 2023
Share this article
0
0 like
_0.jpg?tr=q-80)
Unlike popular belief, diabetes insipidus is not just another type of diabetes. Other than having the same first name and some of the common symptoms, diabetes insipidus, and diabetes mellitus are completely different from each other in terms of causes, effects on the body, and treatments.
Diabetes Mellitus
Diabetes mellitus is a chronic disease that affects the body's ability to produce or use insulin. There are several subtypes of diabetes mellitus, with type 1 and type 2 being the most common.
Type 1 Diabetes: It is an autoimmune disease where the immune system mistakenly attacks and destroys insulin-producing beta cells in the pancreas. As a result, people with type 1 diabetes require insulin injections or an insulin pump to regulate their blood sugar levels.
Type 2 Diabetes: This is a metabolic disorder characterized by insulin resistance, where the body's cells don't respond effectively to insulin. It is often associated with lifestyle factors like obesity and physical inactivity, although genetics also play a role. Type 2 diabetes can typically be managed with lifestyle changes, oral medications, and in some cases, insulin.
Diabetes Insipidus
Diabetes insipidus, on the other hand, is a rare condition that has nothing to do with blood sugar levels. It affects the body's ability to regulate water balance, leading to excessive thirst and urination. There are several types of diabetes insipidus, but the most common is called central diabetes insipidus, which is caused by a deficiency of vasopressin, a hormone that helps the kidneys reabsorb water.
Impact, Causes & Treatment
|
Diabetes Mellitus |
Diabetes Insipidus |
|
|
Impact on the body |
Affects blood sugar regulation |
Affects water balance |
|
Cause |
Body’s inability to produce or utilise insulin |
Issue with making or using vasopressin (or antidiuretic hormone) |
|
Treatment |
medication, diet, and lifestyle changes |
Medications that mimic the action of vasopressin |
Conclusion
Understanding these differences is crucial for accurate diagnosis and effective management. If you or someone you know is experiencing symptoms related to diabetes, it's essential to consult a healthcare professional for a proper evaluation and personalized treatment plan.
Diabetes Management
Leave Comment
Recommended for you
Diabetes Management
Blood Pressure Lowering Medicines May Reduce the Risk of Type 2 Diabetes
Blood pressure-lowering medicines may reduce the risk of developing type 2 diabetes. Some medications, such as ACE inhibitors and ARBs, have shown potential in improving insulin sensitivity and glucose metabolism. By controlling blood pressure levels, these medications may help mitigate the risk and progression of type 2 diabetes in individuals with hypertension.
Diabetes Management
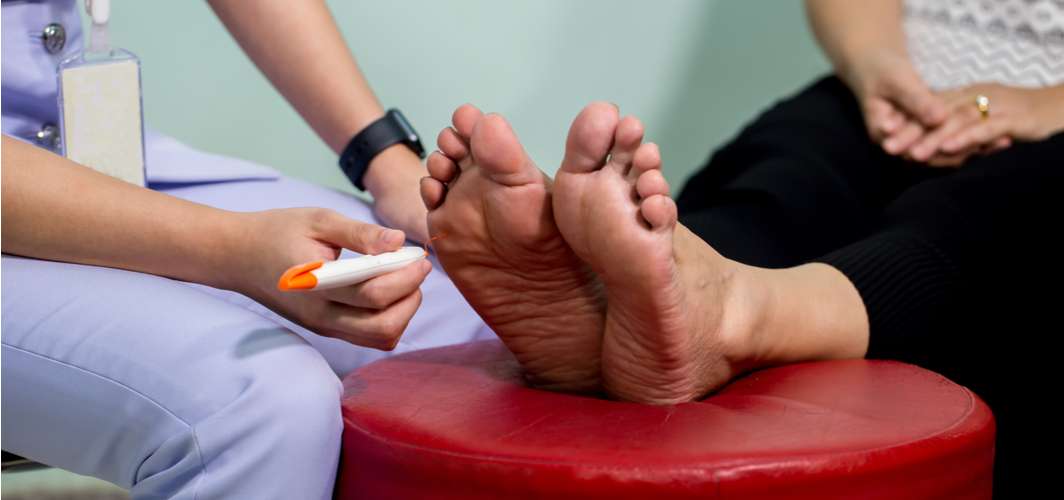
Diabetic Foot: Can it be Prevented?
The development of diabetic foot can be prevented through various measures. Effective prevention includes regular foot care, such as daily inspection and cleaning, wearing comfortable and proper-fitting shoes, managing blood sugar levels, controlling blood pressure and cholesterol, maintaining a healthy lifestyle, avoiding smoking and alcohol consumption, and seeking immediate medical attention for any foot issues.
Diabetes Management
Manage Your Diabetes Like A Pro With Apollo 24|7's 12-Week EMPOWER Programme
Diabetes is one of the most common and widespread lifestyle diseases, affecting millions of people worldwide. Keeping the condition under control is a very challenging task. The Diabetes Management Programme by Apollo 24|7 can help you learn how to manage your condition on your own. Read on to learn how.
Subscribe
Sign up for our free Health Library Daily Newsletter
Get doctor-approved health tips, news, and more.
Visual Stories

8 Fruits That are Incredibly Healthy for Diabetes
Tap to continue exploring
Recommended for you

Diabetes Management
Blood Pressure Lowering Medicines May Reduce the Risk of Type 2 Diabetes
Blood pressure-lowering medicines may reduce the risk of developing type 2 diabetes. Some medications, such as ACE inhibitors and ARBs, have shown potential in improving insulin sensitivity and glucose metabolism. By controlling blood pressure levels, these medications may help mitigate the risk and progression of type 2 diabetes in individuals with hypertension.

Diabetes Management
Diabetic Foot: Can it be Prevented?
The development of diabetic foot can be prevented through various measures. Effective prevention includes regular foot care, such as daily inspection and cleaning, wearing comfortable and proper-fitting shoes, managing blood sugar levels, controlling blood pressure and cholesterol, maintaining a healthy lifestyle, avoiding smoking and alcohol consumption, and seeking immediate medical attention for any foot issues.

Diabetes Management
Manage Your Diabetes Like A Pro With Apollo 24|7's 12-Week EMPOWER Programme
Diabetes is one of the most common and widespread lifestyle diseases, affecting millions of people worldwide. Keeping the condition under control is a very challenging task. The Diabetes Management Programme by Apollo 24|7 can help you learn how to manage your condition on your own. Read on to learn how.